Full Mouth Dental Implant Rehabilitation for Periodontally Compromised Patient
A patient came to us with advanced periodontal disease, a condition where the supporting structures of the teeth progressively deteriorate. Over time, this leads to gum recession, bone loss, tooth mobility, and ultimately tooth loss.
The patient’s primary concerns were difficulty in chewing, discomfort while eating, and a significant loss of confidence due to compromised oral health. Clinical examination confirmed multiple non-restorable teeth with severe bone loss.
Diagnosis & Digital Planning
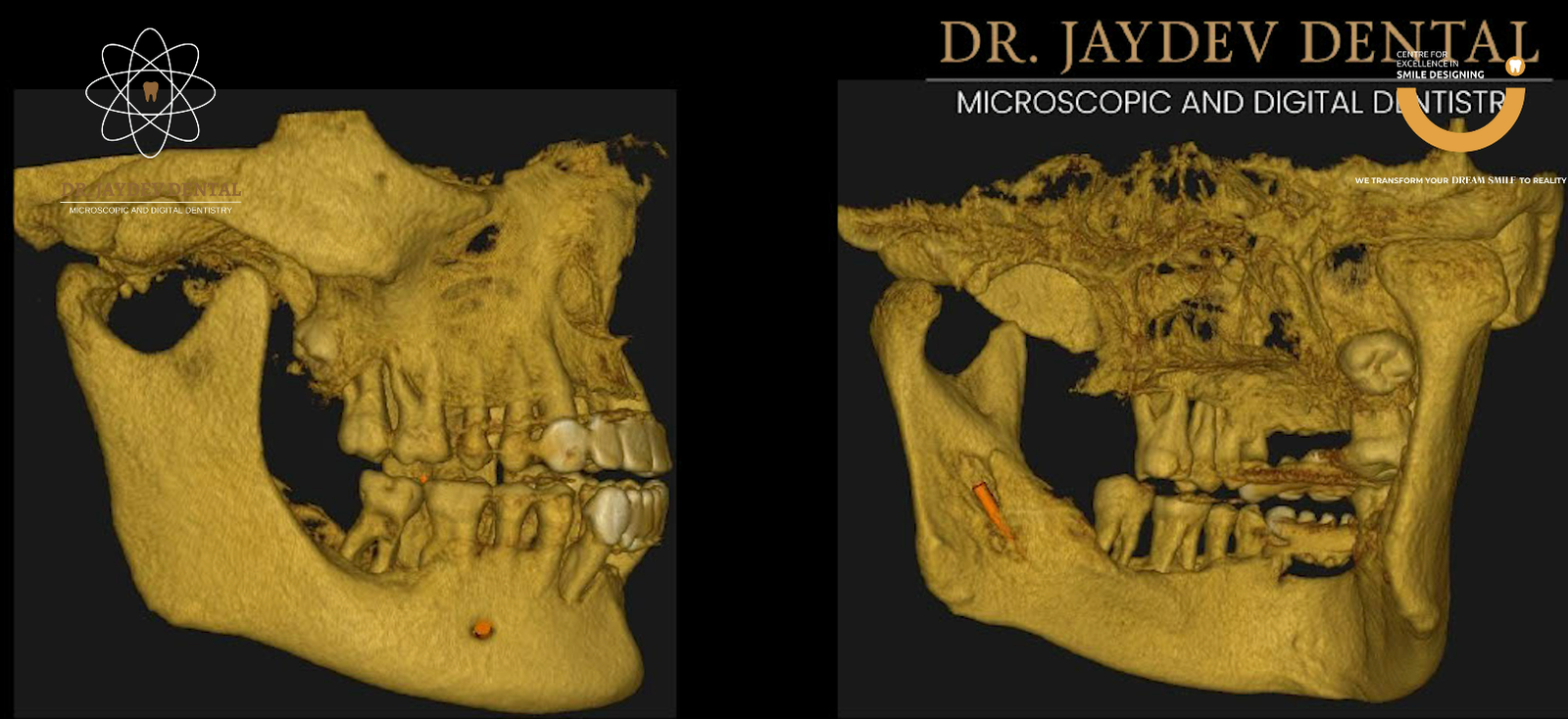
Accurate diagnosis and meticulous planning formed the foundation of this case.
The process included:
- Detailed consultation and chief complaint evaluation
- 3D intraoral scans
- 3D CBCT imaging to assess bone availability
- Virtual implant planning using simulation software
These digital tools allowed precise assessment of:
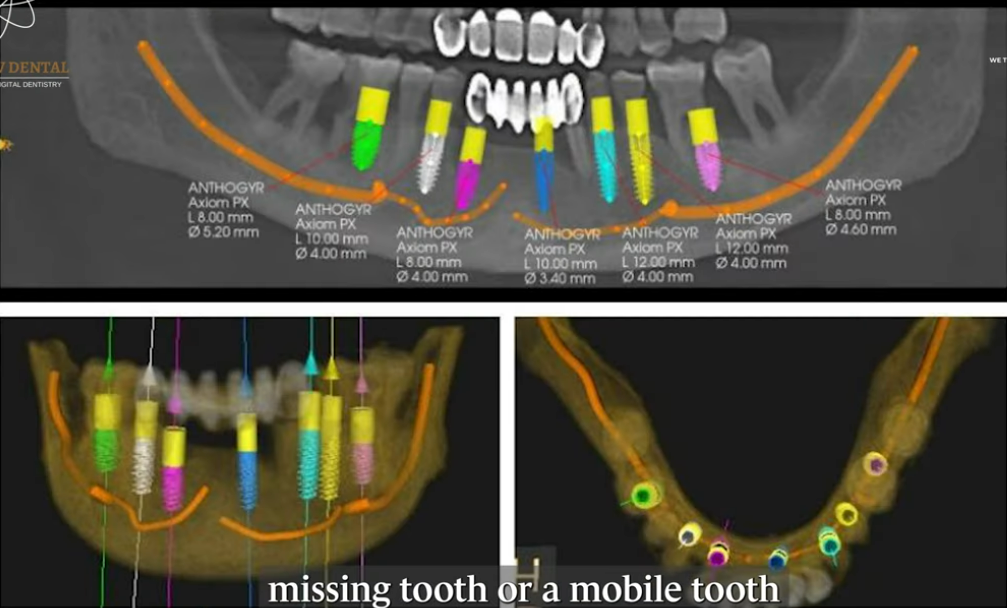
- Available bone structure
- Proximity to nerves and sinuses
- Soft tissue considerations
- Optimal implant positioning
A computer-guided surgical protocol was selected to minimize surgical risk and improve predictability.
Treatment Approach
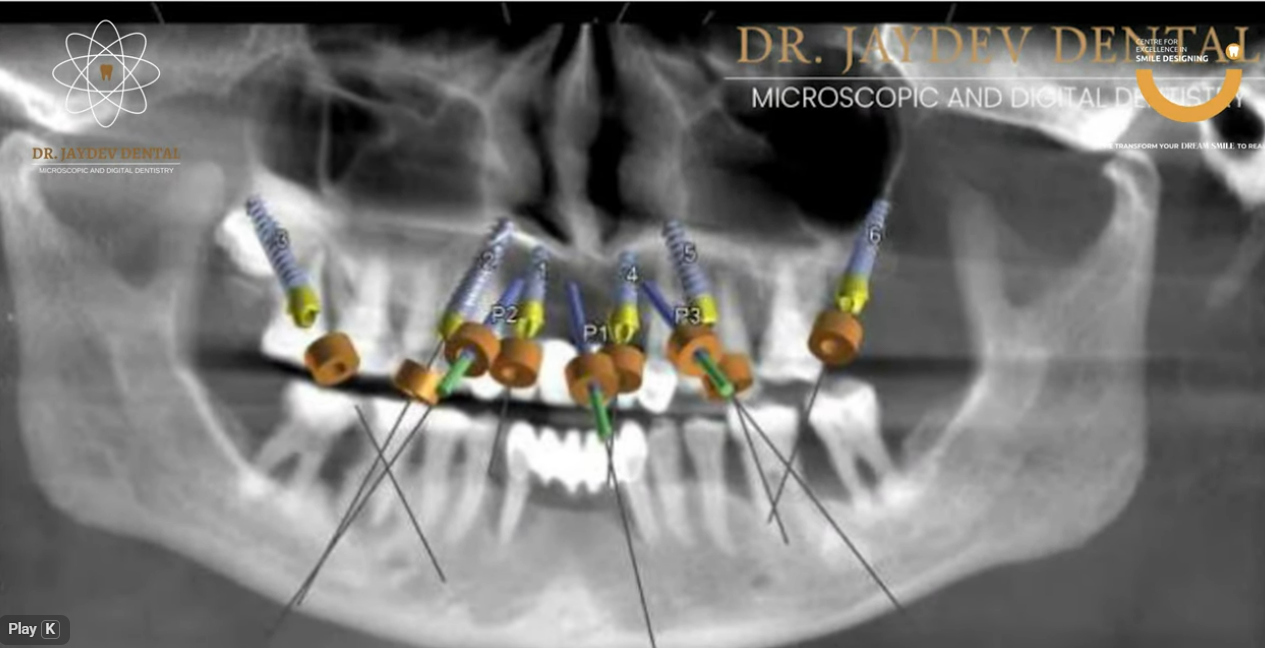
Phase 1: Surgical Phase
All non-restorable teeth were atraumatically extracted.
Using a customized 3D surgical guide, implants were strategically placed through a guided approach rather than relying on conventional freehand methods. This significantly improved accuracy and reduced surgical invasiveness.
The treatment plan included:
- All-on-6 in the maxilla
- All-on-6 in the mandible
A total of twelve implants were placed with precise angulation and depth control.
The use of guided surgery helped:
- Minimize risk of infection
- Reduce the need for extensive bone grafting
- Preserve vital anatomical structures
- Achieve optimal primary stability
Following the surgical phase, a provisional prosthesis was delivered after the initial healing period of 1–2 weeks.
Phase 2: Prosthetic Phase
After a healing period of approximately 3–6 months, during which osseointegration occurred, the implants fused successfully with the jawbone.
Once integration was confirmed:
- Final digital impressions were taken
- A definitive prosthetic framework was fabricated
- Permanent prostheses were delivered
The final restoration provided structural support, aesthetic harmony, and functional efficiency.
Clinical Outcome
The transformation extended beyond dental rehabilitation.
Before treatment, the patient experienced:
- Difficulty chewing
- Persistent discomfort
- Reduced self-esteem
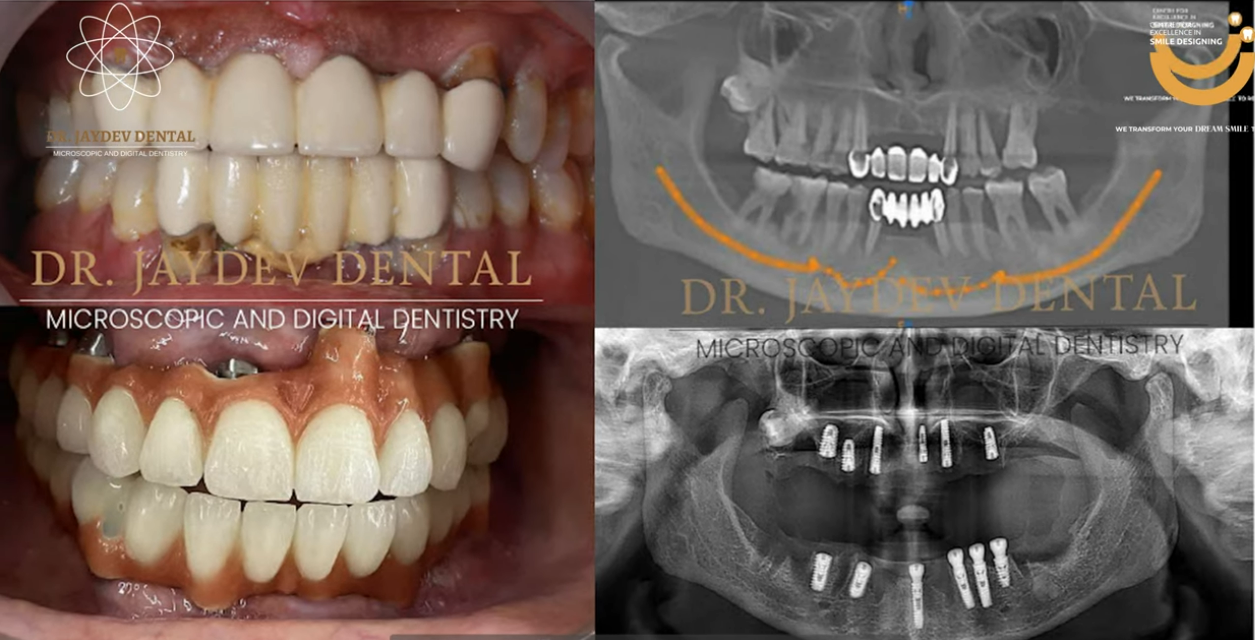
After completion of treatment, the patient regained:
- Stable, fixed teeth
- Comfortable chewing function
- Improved facial support
- Renewed confidence

After completion of treatment, the patient regained:
- Stable, fixed teeth
- Comfortable chewing function
- Improved facial support
- Renewed confidence

